Two articles previously published in this magazine reviewed vaccines for travel: routine, recommended, required, and also outlined the reasons for travel, regions of the world to be visited, and activities posing risk for acquisition of infectious diseases. An overview of drugs for travel contained the same basic framework, but focused on medications to be taken on a trip for prophylaxis or treatment of diseases, whether prescription or OTC, how to pack a medication kit for travel, and how (and if) to purchase medications overseas. This article provides an update on diseases for which there is new information on incidence, vaccines, or drugs. The table provides a short summary of the current state of vaccines and drugs used for prophylaxis of the most common travel-related infectious diseases.
Climate change, urbanization, mass migrations, and poverty have led to the spread of many infectious diseases, especially mosquito-borne and tickborne ones. The Aedes (A. aegypti, A. albopictus) mosquito is ever traveling north and diseases carried by the insect are expected to increase in cooler climes. Waterborne diseases are also susceptible to the effects of climate change and, not surprisingly, are for the most part increasing.

Aedes Mosquito taking a bloodmeal. (cdc.gov)
AVIAN FLU
In April, a man in Texas contracted Avian flu A (H5N1 “bird flu”) from exposure to an infected cow. Most human cases of avian flu result from direct contact with birds that are sick or infected with avian viruses. Symptoms of bird flu range from mild such as eye infection, or upper respiratory symptoms, to severe, including pneumonia, multiorgan failure, and death. Even though humans have been exposed to and infected by bird flus for over 20 years, this is only the second animal-to-human transmission reported in the US (and the first by a non-bird); this is one to keep a very close eye on. There is no vaccine available for prevention.
CHIKUNGUNYA
The chikungunya virus, spread by the Aedes mosquito, causes disease that is characterized by severe arthralgias (aka “bent over in pain”). Prevalent mainly in tropical and subtropical parts of the world, recurrent global outbreaks have affected thousands of US travelers withsmall numbers of casesreportedthroughout the US. In November 2023, the US FDA approved IXCHIQ, the first vaccine for prevention of chikungunya, for travelers >18 years old going to a country or territory with a current outbreak. It is not available in pharmacies yet.
DENGUE
The dengue virus is the most commonly spread infection by Aedes mosquitoes and causes 100-500 million cases annually worldwide. The infection, aka “breakbone fever,” can result in serious disease (especially when contracted for the second time) resulting in hospitalization and death. As of early April, there were 846 cases of dengue reported in the US and its territories so far in 2024. Over 60% of these were locally acquired (meaning the spread of the disease is occurring within residents of the country or state); the rest were brought back from travel to another area. Most of these local cases have occurred in Puerto Rico, prompting the territory's Department of Health to issue a Public Health Emergency. In the US, local spread has been reported in Florida, Hawaii, Texas, Arizona, and California. A vaccine (Dengvaxia) was recently approved for dengue prevention in the US, but only for children 9-16 years old living in endemic areas (not for travelers yet). Dengavaxia and another vaccine (Qdenga) are available in endemic countries for more widespread use. See this recent story about dengue in Wilderness Medicine Magazine.
LYME DISEASE
In addition to climate change, Lyme (and other tickborne) infections continue to rise due to encroachment upon tick habitats and increased reporting requirements for the disease. It’s estimated that nearly half a million people in the US contract Lyme disease every year, and the Lyme ticks abound in forested areas of Europe as well. LYMERix® vaccine was discontinued in 2002 and anyone who received that vaccine is no longer protected. A new Borrelia subunit vaccine currently in Phase III trials and a monoclonal antibody are being developed for Lyme disease prophylaxis. Dogs have a vaccine (cats don’t get Lyme!), so why not humans?
MEASLES
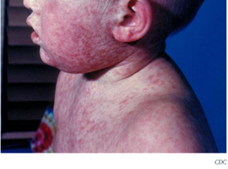
Child with measles rash. (cdc.gov)
Measles was eradicated in the US in 2000, but lower vaccination rates, especially during the COVID-19 pandemic, has led to outbreaks in the US and globally. From January to March of this year, 58 cases of measles have been reported in the US, mostly in unvaccinated travelers to other countries. As one person with measles can infect 90% of unvaccinated persons, this virus is highly transmissible, but very easily prevented with vaccination. The CDC issued an advisory in March 2024 for all persons >6 months of age living in the US and traveling internationally to be current on their measles, mumps, rubella (MMR) vaccine series.
MENINGOCOCCAL DISEASE
An alarming increase in the numbers of invasive disease caused by Neisseria meningitidis serogroup Y is occurring in the US, prompting a CDC Health Alert Network (HAN) Health Advisory. The disease is preventable by vaccination (MenACWY) and is recommended in the US for pre-adolescents (11-12 yo) and adolescents and some adult groups with risk factors. The MenB vaccine is also recommended for young people with certain risk factors. The vaccine is also recommended for travelers to countries with endemic meningococcal disease.
PERTUSSIS
Lethal outbreaks of pertussis are occurring all over the world now, including a cluster of cases recently in Hawaii. This respiratory disease is especially serious in infants and children, but is increasingly affecting adults who have waning immunity from vaccination. Travelers are recommended to keep current on their Tdap (tetanus, diphtheria, pertussis) boosters every 10 years.
POLIO
Despite longstanding attempts to wipe polio off the face of the earth and getting oh-so-close, some strains of the disease persist. The US Advisory Committee on Immunization Practices (ACIP) recently updated the general recommendations for polio vaccine to encourage all those at risk of polio infection because they are not fully vaccinated and live in a community where poliovirus is circulating to get vaccinated as soon as possible. Most people in the US are assumed to be fully vaccinated with injectable polio vaccine as it is a routine childhood vaccine, but this is not always the case.
ZIKA
Interestingly, the number of Zika cases have plummeted since an outbreak of Zika in 2016 caused 5,000 cases of the disease in the US and many more in South America (especially Brazil). There were only five cases in the US in 2022, all travel-related, which is good news, as the numbers are not high enough to cause local acquisition. The major concern with Zika is a woman contracting the disease during pregnancy; during 2016-2017, over 2600 cases of birth defects were attributed to Zika infection. There is no vaccine for Zika.
ALTITUDE ILLNESS
Not an infectious disease, but with updated recommendations for drug prophylaxis and treatment of AMS, HACE, and HAPE, WMS recently published “Wilderness Medical Society Clinical Practice Guidelines for the Prevention, Diagnosis, and Treatment of Acute Altitude Illness: 2024 Update.” See discussion and tables for updated drug choices.
See the list below of common infectious diseases for which there is vaccine or drug prophylaxis and those for which there is not. Many of the preventable and non-preventable diseases have treatment options available; they are not listed here. For all diseases, the usual insect, food/beverage, respiratory, contact, and bite avoidance precautions apply, whether or not there is prophylaxis available. Note that some routine vaccinations are not listed here (HPV, Hib, etc.); persons who plan to travel should be current on all recommended vaccine schedules.
Whether you’re traveling for fun, work, mission, research, military deployment, etc. – make sure you are fully protected against hazards, including vaccines (and in plenty of time before leaving), a well-stocked medical kit, and a full fund of knowledge.
TRAVEL-RELATED INFECTIOUS DISEASES
Mosquito-borne 🦟
• Vaccine/Drug Prophylaxis:
• Japanese encephalitis
• Malaria
• Yellow Fever
• No Vaccine/Drug Prophylaxis:
• Chikungunya
• Dengue
• West Nile Virus
• Zika
Tickborne 🕷️
• Vaccine/Drug Prophylaxis
• Tickborne Encephalitis
• No Vaccine/Drug Prophylaxis:
• Lyme (PEP* recs from CDC)
• Rickettsial diseases (e.g., Rocky Mountain Spotted Fever)
Food/Water 🥘
• Vaccine/Drug Prophylaxis:
• Cholera
• Hepatitis A
• Leptospirosis
• Travelers’ Diarrhea
• Typhoid Fever
• No Vaccine/Drug Prophylaxis:
• Cryptosporidiosis
• Giardiasis
• Norovirus
Respiratory/Airborne 🌬️
• Vaccine/Drug Prophylaxis:
• COVID-19
• Diphtheria/pertussis (Tdap)
• Influenza
• Measles/Mumps/Rubella (MMR)
• Meningococcal
• Pneumococcal disease
• No Vaccine/Drug Prophylaxis:
• Coccidiomycosis
• Histoplasmosis
Contact 🤝
• Vaccine/Drug Prophylaxis:
• Hepatitis B
• Polio
• Varicella
• No Vaccine/Drug Prophylaxis:
• Hepatitis C
• HIV
Bites/Wounds 🩹
• Vaccine/Drug Prophylaxis:
• Tetanus (Tdap)
• No Vaccine/Drug Prophylaxis:
• Rabies (PEP*)
• Many!
*PEP = post-exposure prophylaxis
Visit the CDC’s Travelers’ Health page for the most current recommendations.

The CDC Yellow Book, updated for 2024, is also an excellent resource.
