The WMS was excited to head to Canada to host its 2024 Winter Conference in Whistler, British Columbia in March. This year’s conference included 545 in-person and virtual attendees from 15 different countries. Below we hear from the Student and Resident Ambassadors on their first-time experiences at a WMS conference!
As a medical student on the East Coast, I often found myself reaching far distances in search of wilderness medicine opportunities. Imagine my delight upon joining the milieu at the WMS 2024 Winter Conference and finding passion for the field overflowing from every attendee I spoke with: physicians engaged in everything from climate medicine to naval diving, graduate students researching thermal heat transfer in arctic conditions, future APP’s delivering lectures on the realities of fighting wildland fire. What an amazing collaboration opportunity this conference provided, stimulating the flow of knowledge and ideas with medical professionals from across the globe. The incredibly welcoming atmosphere was strikingly different from the oft rigid hierarchies found in a hospital setting. As a first-time attendee, I wasn’t sure what environment I would find upon arrival. However, within seconds of sitting down to breakfast the first morning, my uncertainty was assuaged. MDs, APPs, and students of all kinds swapped stories from the prior ski day and discussed the latest paper on the efficacy of maple syrup as an ultrasound gel. I can’t imagine a better way to continue breaking down interdisciplinary barriers than a shared passion for wilderness medicine and pancakes.
Before lectures each day, the hall was sprinkled with children of the attendees, yet for a change, all the kids went out to shred the slopes of Whistler while the parents stayed indoors to learn. The conference featured an amazing line up of lectures from “Cave Rescue” to “Risk and Decision Making” to “Surfer’s Myelopathy”. The record attendance for this conference led to lively post-lecture discussions; without moderator intervention I’m sure we would have run several hours over time. Additionally, there were unique smaller group workshops, covering topics from ultrasound to ice axe self-arrest to designing medical student electives, providing more hands-on and discussion-based learning opportunities.
I had an amazing time at this year’s WMS Winter Conference; the connections I made and knowledge gained are invaluable. I’m already looking forward to the next one!
-Kirra Paulus, MS-IV

Left: Preparing for Ice Axe Self Arrest Workshop (Kirra Paulus)
Right: Gathering for exhibitor presentations during lunch breaks (Kirra Paulus)
Several feet of snow! That was the forecast for the 2024 WMS Winter Conference in Whistler and wow did it live up to the expectations. With this beautiful backdrop, a wide variety of presentations and workshops would take place over the next three days.
The first day included lectures such as “Psychological First Aid for Responders”, which looked at delivering more data-guided practices to some of the most traumatic aspects of wilderness medicine and rescue. I learned to replace outdated techniques such as “debriefing” and large group meetings as they can actually increase secondhand trauma and create more victims in the long run. There were also specific actions such as the 3-3-3 follow-up method and accessible screening tools which allow us to better care for each other. “Solar Exposures in Wilderness Dermatology” also struck a chord with images of common skin rashes to graphic malignancies and resections. Importantly, it also went over how we can protect ourselves in the outdoors with a combination of sun protective clothing, wide brimmed hats, and sunscreen. I also loved the idea of a dermatologic first aid kit and will be building one for my next trip.
The afternoons were spent in small group workshops learning the basics of ultrasound and how to apply it in wilderness settings. We went over many of the common scenarios a provider may see and the ultrasound exams that would be beneficial to treating their patients. I was especially interested in the breadth of participants and the locations and situations they work in- from rural critical access hospitals, to flight teams on helicopters, to EMS crews, to primary practice clinics. The next day built on these exams and added gamification to test skill. A blind, timed FAST had voices rising and ultrasound jelly everywhere. The workshop also had the full gambit of devices from handheld “personal” ultrasounds to hundred-thousand-dollar all-in-one solutions which let members test out the current market before deciding to buy.
As the conferenced closed, it was a wonderful few days of learning, chatting, and snow. This was my first WMS conference but after meeting so many incredible individuals I am excited for the next!
-James Whall, MD

Left: POCUS Workshop with Tatiana Havryliuk, MD (Kirra Paulus)
Right: Conference Introduction by Arun Ganti, MD (Kirra Paulus)
As I handed out badges the first night of the conference still dressed in my ski clothes, I began to realize, this was like no other medical conference. Physicians, APPs, paramedics, and more filled the atrium in their own ski gear and winter coats, some with patches highlighting SAR teams and expeditions. I watched them hug and laugh, recounting adventures since they last spoke. This was the medical community I had been dreaming of this year while during my learning-packed but often hierarchical and formal third year rotations.
In reflecting on what I learned throughout the week, I found a common thread: the duality of patient and provider in the wilderness setting. Josie Heath, paramedic and PA student spoke about one potential obstacle when treating wildland firefighters such as herself: the mentality of being tough and not asking for medical help. I would guess that this applies to many of us in the wilderness medicine community. We learn about pathologies and injuries in the outdoors, and although we’d like to separate these from our own realm of possibility, it is more difficult than in the hospital setting where we are not necessarily enjoying the same activities as our patients.
Dr. Miles McDonough introduced the term “lateral emotional driver” when speaking about his own case study of being rescued while climbing Mt. Stuart – an aspect not often taken into consideration when discussing risk and decision-making in mountain rescue. Dr. Brendan Byrne added another dimension to this in his talk about naval medicine, proposing that “the risk matrix changes in work vs. play” and teaching the green/amber/red model of assessing risk and responder capability. This same concept was touched on in Dr. Roger Mortimer’s lecture on psychological first aid. We learned that thoughts of “it could have been me” can itself lead to PTSD even when the event was not personally experienced.
We also learned strategies to help teams through these events. This is what makes the WMS so wonderful, a group of like-minded people making the activities that they love safer. During Dr. Maya Stawnychy’s talk on surfer’s myelopathy, I pondered if I might experience this condition myself as a novice surfer. Simultaneously, I took note of the imaging findings in case I see it in the ED someday. I gained a tremendous amount of clinical and outdoors knowledge from this conference, and I’m inspired to keep learning!
-Thea Lance, MS-III
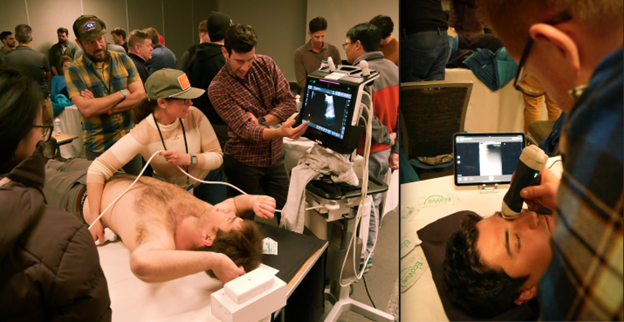
Left: POCUS Workshop guided by Neil Krulewitz, DO (Kirra Paulus)
Right: More POCUS practice by attendees (Kirra Paulus)
Touching down at the YVR airport in the morning on March 10, everything felt familiar. I spent three great years in Vancouver at the University of British Columbia, and I relish any chance to come back for a visit. I took the Skytrain downtown to Burrard and hopped on the shuttle. The views on the Sea to Sky Highway were also familiar, although they never get old no matter how many times I drive the road up to Whistler. But the familiarity ended as I made my way over to the Whistler Conference Centre for the start of the WMS Winter Conference. Being a med student from a smaller city in Ontario, I’d had little prior exposure to this community. I was a bit nervous, but once people started arriving in ski boots to pick up their nametags, my nerves quickly faded. Over the course of the next four days, I learned a ton about this field and met some fascinating people.
A couple of things seemed particularly important to me:
- Interdisciplinary collaboration: At school our dean talks to us a lot about how important it is to work across disciplines in healthcare; this conference was the first time I had seen it happen so perfectly in practice. I met paramedics, nurse practitioners, family physicians, specialists, residents, PAs, and others, all coming together around this common interest of providing medical care in remote and wild environments.
- Wide breadth of practice and expertise: Before this conference, I’d had little to no exposure to wilderness medicine as a discipline. I think what surprised me most was how many avenues there are to incorporate wilderness medicine into a career path. It’s exciting how incredibly broad the field is. It can include anything from administering blood transfusions 1000m underground (as outlined by Dr. Mortimer in his lecture about the 2022 Turkish cave rescue) to advocating on a systems level for improved climate emergency preparedness (as described by Dr. Vohra in his lecture “Global Health in a Changing Climate”). I left feeling excited about all the ways I might be able to get involved with this community in the future. I’m extremely grateful for the opportunity to attend this conference and I’m even more grateful that it snowed- and everybody got to experience a bit of Pacific Northwest powder!
-Amelia Boughn, MS-III