In the original installment of Base Camp Rx, "The Right Stuff," I introduced a framework for thinking about medications used for prevention or treatment of hazards in wilderness environments . Now we're going to discuss the effect of wilderness environmental conditions on medications that are being taken for a pre-existing condition. This information can be especially useful if you are affiliated with an organization that requires a participant medical history or health questionnaire . An example of this type of form is used by NOLS. At a minimum, someone involved in wilderness activities (especially if on an organized trip) and taking medications should know the following: 1) the name of their medication(s), 2) the dosage (or at least how many times a day they take it), 3) what they are taking it for, and 4) the name of the prescriber. It's also helpful to know how long they have been on it if they are taking it regularly. The key point is to make sure they have it on the trip with them! It's amazing how many of these criteria are not fulfilled.
This column will not cover medications carried by the expedition or trip leader that are administered for illness or injury during a trip (a subject of a future column), or the effect of environmental conditions on the storage of drugs (discussed in a previous column, "Medication Transport in the Wilderness").

Altitude
Traveling to higher altitudes can have many effects on the respiratory and circulatory systems, multiplied by the effect of solar radiation and dehydration. An interesting study was reported in 1932 of the increased toxic potential of digitalis (digoxin) at higher altitudes in cats and pigeons, which was bad news for felines and fowl with heart failure (1). A more current study found no diminishment of performance of metered dose inhalers (MDIs) – good news for those with asthma, although the study was not done in real people, but with an "Idealized Throat." (2) In another study, type 1 diabetics who trekked to extreme altitude (>5,000m) were found to have increased insulin requirements, thought to be attributable to hyperglycemia associated with AMS; these results corroborated that of several other reports. (3)
1. Leake CD. Effect of Altitude on Drug Action. Cal West Med. 1933 Mar; 38(3): 188.
2. Titosky JTF et al. The Effect of Altitude on Inhaler Performance Journal of Pharmaceutical Sciences Volume 103, Issue 7, pages 2116–2124, July 2014
3. deMol P et al. Increased insulin requirements during exercise at very high altitude in type 1 diabetes. Diabetes Care. 2011 Mar;34(3):591-5. doi: 10.2337/dc10-2015. Epub 2011 Jan 27.

Sun
Certain drugs can cause a photosensitivity or phototoxic reaction in persons who do not protect themselves from the sun by staying out of it or wearing sunscreen or protective clothing (or not taking the medication if they can't avoid sun exposure). Reactions can look like a very bad sunburn or other types of allergic reactions with pruritus, erythema, macules, papules or vesicles. I knew a doctor a number of years ago who used to come into the pharmacy with a prescription for tetracycline that he wrote for himself every time he went on a tropical vacation so he could always maintain that perennial glow (this was before self-tanning products); I don't recommend this. Spilling a margarita on yourself at poolside can also cause this type of reaction—some citrus fruits like lemon and lime are topically phototoxic.
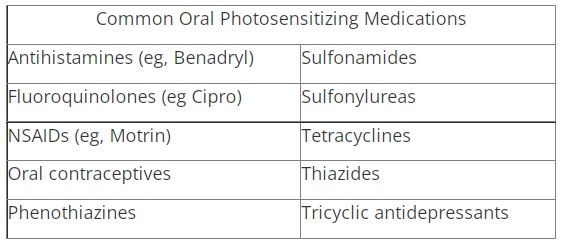
From: Krakowski AC. Exposure to Radiation from the Sun. Chapter 14. In: Auerbach PS, ed. Wilderness Medicine. 6th ed. Philadelphia, PA: Elsevier Mosby; 2012:311-312.

Desert/ Heat/Dehydration
Some drugs can exacerbate heat illnesses in environments that can be extremely hot, such as the desert, by interfering with the body's ability to dissipate heat. Others can do this by causing dehydration.
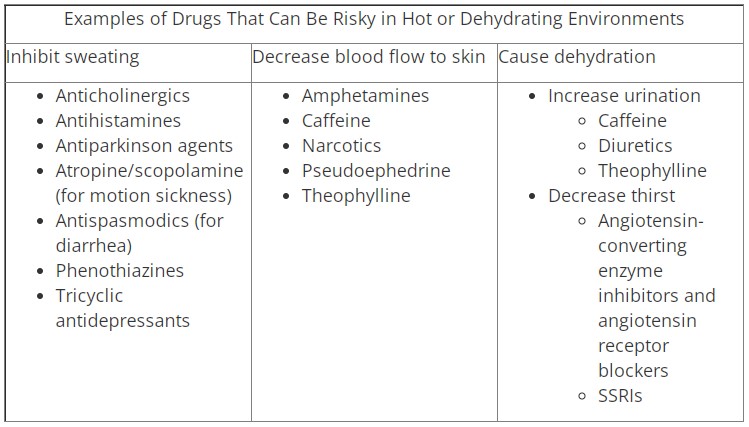
References: Martinez M, et al. Drug-Associated Heat Stroke. South Med J 2002.95:799-802; Summer Heat Can Put You at Risk! http://netwellness.org /healthtopics/pharmacyw18.cfm; Walter AN. Hydration and Medication Use. Am J Lifestyle Med. 2011;5(4):332-335.
Dehydration itself causes risks, occurring with excessive exertion, in the desert, at altitude, in extremely humid environments, etc. Nonsteroidal anti-inflammatory agents (NSAIDs) are known to cause damage to the kidneys in the setting of dehydration. Often their use as a treatment for muscle pain is discouraged if excessive fluid losses are expected to occur. In any setting of dehydration, you shouldn't take your Vitamin I if you don't fill your tank first!

Flying
For tips on how to package and transport medications on a flight, see "Medication Transport in the Wilderness," mentioned above. Observe the commandment: Thou shalt not pack important medication in your checked baggage (or you may die). Maybe not expire, but be very uncomfortable, or give the very marginally trained flight crew or fellow volunteer medical HCP passenger a scare. While your plane cruises at an altitude of 35,000ft (10,600m), the cabin is pressurized at ~5,000-8,000ft (~1,500-2,400m), a medium-high altitude, with attendant low humidity. While there isn't a specific list of medications specifically contraindicated for flying, there are medical conditions that require medical clearance. More information can be found in the IATA (International Air Transport Association) Medical Manual. For airmen (not sure about airwomen), the FAA issues an extensive list of medications that should not be on board in a pilot's body while he or she is operating aircraft.

Diving
There are waves of information on the internet about drugs and diving from organizations such as DAN, PADI, NAUI, and dive doctors, such as this site.
Diving to a certain depth, or the mixture of gas a diver is breathing, could potentially have effects on a medication (including recreational drugs and alcohol). More importantly, the person's underlying medical condition that is being treated with the medication should be considered as to whether or not it is prudent to dive (and in some cases, directly proportional to the amount of money spent on the expensive dive trip).
WMS offers this sensible advice:
- Whenever possible, avoid all drugs when diving
- Any medication that impairs mental judgment or physical capacity should be very carefully considered before being used when diving. If the medication is used, the expected benefits of its use should outweigh its risks
- Never take a drug for the first time before diving
- Always consider whether the reason for taking a drug is reason itself not to dive
- Always consider the known side effects of a drug and whether those would be a problem when diving
Reference: Van Hoesen KB et al. Diving Medicine. Chapter 77. In: Auerbach PS, ed. Wilderness Medicine. 6th ed. Philadelphia, PA: Elsevier Mosby; 2012:1546-7.
Cold
There is not much information on the effect of medications in cold environments. WMS stated in their 2014 hypothermia guidelines that many drugs and medications suppress shivering, thereby complicating the classification of hypothermia. Usually, only one round of ACLS drugs are recommended in the case of cardiac arrest in profound hypothermia.
Drugs that cause poor circulation may contribute to the development of frostbite.
Reference (hypothermia): Zafren K et al. Wilderness Medical Society practice guidelines for the out-of-hospital evaluation and treatment of accidental hypothermia: 2014 update.
Wilderness Environ Med. 2014 Dec;25(4 Suppl):S66-85.
Posted on August 11, 2015