Madagascar – one of the world’s poorest countries with some of the most exotic wildlife on the planet, far from home, and with a predominantly young population. An ideal destination for a medical mission for a budding pediatrician interested in remote medicine. I first came across the US-based charity organization, International Medical Relief (IMR), via colleagues during the WMS-endorsed Tropical, Travel, and Expedition Medicine Skills Course (TTEMS) organized by the College of Remote and Offshore Medicine. IMR offers a range of short medical missions across the globe, of which Madagascar immediately appealed to me.
Pre-trip Preparation
Preliminary research on Madagascar, a large island nation off the southeast coast of the African continent, combined with a useful predeparture checklist from IMR helped organize my preparations. I ensured I had copies of documentation for visa purposes (to be issued on arrival), copies of my medical certification, IMR correspondence confirming my part as a mission team member, and that digital versions of all of these were always at hand on an accessible USB drive. Personal health considerations included an initial vaccination check with our national vaccination services, procurement of less commonly available WHO-recommended immunizations such as rabies, anti-malarial measures in the forms of malarone and DEET repellent sprays, and packing long sleeved, light colored clothes to deter mosquitos. I also put together a comprehensive medical kit for my own personal use, comprising of analgesics, antiemetics, antidiarrheal agents, decongestants, oral rehydration salts, wound care options, and antibiotics. I was very much aware that access to medical care so far from home would be challenging should I become unwell. I also invested in travel insurance including coverage for repatriation if needed and two means of water purification: a water filtration bottle using an activated charcoal filter, and sodium dichloroisocyanurate water purification tablets.
Clinical Experiences
We first set up a base in Tamatave, a city on the eastern coast, after a fourteen hour drive from the capital Antananarivo. After resting for the night, we set off along the Pangalan Canal in a small boat for another two hours, before reaching our destination of a small village on the banks of the canal. We would set up a clinic here for two days.
Toasamina, on the eastern coast of Madagascar. (Google Maps)
The clinical case mix varied from acute conditions like respiratory tract infections or gastroenteritis, to more chronic conditions like the sinister signs of pediatric failure to thrive. One child, a two-year-old girl, came to the clinic with her mother as she had not been growing. She had a resting tachypnea and was generally small for her age. Examination revealed a loud pansystolic murmur at the lower left edge of her sternum, along with hepatomegaly - signs suggestive of congenital cardiac disease with worsening heart function. There was little that could be done by a visiting doctor other than referring to the local tertiary center in Tranom Pasalama – without proper diagnostics, treatments, and likely urgent surgical intervention, this would be a life-limiting condition.
Over two days I saw over fifty children with a variety of acute and chronic complaints, ranging from acute infections to developmental delay in infants born prematurely, lots of dental disease, and plenty of scabies. The golden rule of the mission- “don’t hug the babies”- was a poignant one, though one I had learned before during my pediatric training in Malta when receiving migrant children who had just made the perilous journey overseas from the north coast of Africa. I came to understand and appreciate the limitations of remote clinical practice and the limited long term changes that acute medical interventions from shorter missions like ours could make. The real, lasting changes from our visit came from community education sessions on topics such as hygiene, first aid, and dental care.
Our second clinic came in the form of a local school, with a large school hall repurposed for our visit. I saw over 100 children in one very long day, treating large numbers of ascariasis and respiratory tract infections as well as other minor complaints. We ran out of antiparasitic medications towards the end of the day, with our medical lead leaving us to source more medication supplies from local pharmacies.

The morning view from our clinical station at 09:00. (Jamie Grech)
An 11-month old child presented with irritability, vomiting, and lethargy – potential signs of a CNS infection- leading to a stat IV fluid bolus and high dose ceftriaxone administration before urgent referral to the local hospital, the Christian mission facility at Bethany Hospital. A young infant of three months was also referred there urgently with a massive incarcerated inguinal hernia at serious risk of strangulation. A pro bono repair was organized by the mission team, as his parents could not afford the hospital or surgical fees.
On the second day here, I saw over sixty children: many minor complaints again, with serious illnesses hidden between the well-appearing patients- a universal a theme in modern emergency departments as well as in a small make-do remote medicine clinic in Madagascar. One little three-year-old girl had a serious lower respiratory tract infection in the setting of a clearly undiagnosed neuromuscular disorder: extreme lordoscoliosis, failure to thrive, global developmental delay, and bilateral club feet. Respiratory infections are a serious complication of such chest wall anomalies – she would require a full multidisciplinary team review and even a genetic workup if seen in the developed world. A newborn with likely late onset neonatal sepsis presented with high-grade fever at 26 days of life – urgent referral for a sepsis screen led me to discover that CSF samples were only taken once a week, according to laboratory availabilities. Initial antibiotics were given, but further inpatient care would be needed. She was also referred to Bethany Hospital, for as comprehensive a sepsis screen as was possible and continuation of IV antibiotics.
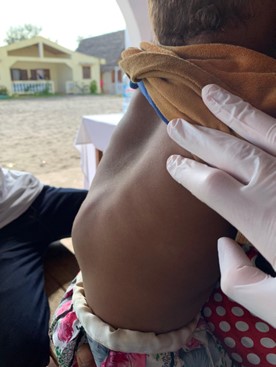
Severe lordoscoliosis. (Jamie Grech)
A universal challenge during all patient contact was the language barrier. Local interpreters for Malagasy and its dialects were on hand, but the concerns of a parent could be diluted when not heard directly in their own language. Reading my journals of patient interactions after returning to home soil in Malta has left me with a great sense of awe, wonder, and an element of helplessness. The diverse presentations and assortment of clinical conditions was truly a challenge to manage with limited provisions for any healthcare provider.
In Part 2, Dr. Grech will discuss his experiences working in a Madascan prison and his takeaways from his global health experiences.