
Across 17 days, with 12 trekkers, three Everest ER docs, seven sherpas, porters and yaks, we set out on the trek of a lifetime to Everest Base Camp (EBC), learning wilderness medicine in many ways. Like all successful adventures, ours began with preparation. We prepped at home by reading about the region, gearing up and checking in with our travel medicine folks. This was followed by a gear check and orientation with Wongchu Sherpa and the Peak Promotions gang in Kathmandu. We had a practical talk on wilderness medicine kits at the Yak & Yeti Hotel, resulting in a mad rush to the local pharmacy - which resembled a coffee bodega in New York City - to obtain medications that would be used liberally over the next three weeks. Then we were off!


Our preparation for our adventure included a standard gear check and a trip to the local pharmacy for medications.

Loading up the Yak & Yeti as we prepare to board the plane.
The first flight out of Kathmandu to Lukla was delayed, so we began learning about acclimatization at the airport. Just as the group began a heated discussion about who would acclimatize, and who knew if they had a PFO (Patent Foramen Ovale), it was time to jump on the plane for an exhilarating flight into Lukla.

Following a delay at the airport, we were exhilarated to finally be on our way to Lukla!
Over the course of our 17-day trek to EBC, five out of 15 trekkers developed Traveler's Diarrhea (TD, or "D & V" as our United Kingdom friends affectionately call the most common symptoms), including one trekker on night one. Generally, these trekkers required just an extra night to recover and replenish once they began taking antibiotics - usually azithromycin. We had learned that 80 percent of diarrhea among visitors to the Khumbu is bacterial. We encouraged early treatment with heavy emphasis on the rehydration solution. As it turned out, our 33 percent TD rate was quite good compared to the 75-90 percent TD rate among other trekking groups we met along the trail. I attribute this partly to our aggressive sharing of hygiene skills.
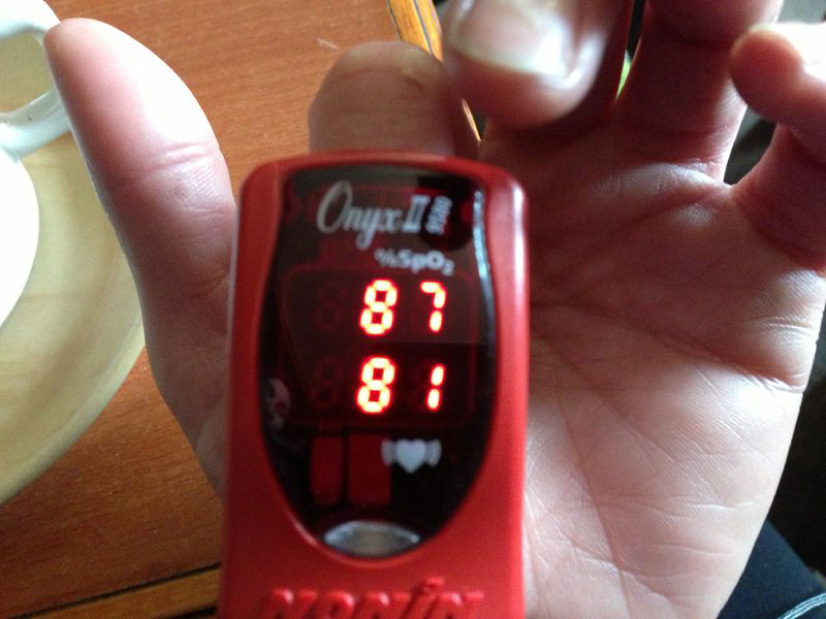
Our trip leader's oxygen meter gave us a good indication of the type of environment we were dealing with.
Half of the trekkers took acetazolamide prophylactically from the onset. Some participated in Dr. Scott McIntosh's research protocol comparing different doses for prevention. By the time we reached Gorakshep (5171 meters), 12 of us were taking acetazolamide for AMS (acute mountain sickness). Some had to increase their dose from prevention dose to treatment dose with the onset of a high altitude headache (HAH) that did not resolve with NSAIDs (non-steroidal anti-inflammatory drugs). Of the three not taking acetazolamide, one had a high altitude headache that resolved with NSAIDs.
We were lucky enough to trek up with the three Everest ER Docs for the season: Suzi Mackenzie, Pranav Koirala and Kirsty Watson, who made tremendous contributions to our lectures, discussions and management of the groups' medical issues. Hypoxia and acclimatization came up multiple times a day for obvious reasons.

Our three Everest ER doctors provided invaluable contributions to our lectures, discussions and the overall success of our adventure.
Two trekkers required helicopter rescues from the trail. The following are case descriptions for those two trekkers.
Case #1:
John, a 63-year-old male, had a history of HTN (hypertension), as well as back surgery 15 months prior to the trek, with minor baseline gait instability, which had been treated with physical therapy. On the trail, John accommodated nicely with trekking poles and assistance when necessary from Chhongnuri Sherpa. John did quite well and looked strong up until Lobuche (4930 meters) when his HAH did not respond to NSAIDs. John stayed an extra night in Lobuche and made it to Gorakshep, the last tea house before EBC.
At Gorakshep, John developed TD. Chhongnuri stayed with him and encouraged fluids, but even so, John could not keep up with the gastrointestinal losses. It was clear by the next day, even though there was some improvement with fluids, John would not be able to trek on to EBC. John's condition worsened overnight when he became unable to push fluids. After a brief discussion that morning, Wongchu Sherpa arranged a helicopter as the group began our descent from EBC. We intercepted John at Gorakshep prior to his med-evac. John was febrile, his dehydration severe, his HAH was back at 10/10, he was short of breath, had orthopnea, and a Pox of 75 percent. When he got up to use the restroom, John fell. It's unclear whether the fall was due to HACE (high altitude cerebra edema) or dehydration in the setting of some baseline gait instability. Given the fact that we were at extreme elevation, we treated John for HAPE (high altitude pulmonary edema) and HACE prior to getting on the chopper. We also started a second antibiotic. John reported that his HAH and shortness of breath resolved as the chopper landed in Kathmandu.
Take-home point: descent is the definitive treatment for HAPE and HACE.

We did what we could to treat John for HACE and HAPE, but descent proved to be the definitive treatment.
After six liters of IV fluids, John was discharged from the CIWEC clinic to the Yak & Yeti, where he waited for us to celebrate the accomplishment of trekking in the Khumbu. John felt thrilled to be healthy and comfortable, and we are all proud of the trek that he made. Wongchu arranged a delightful final banquet in Kathmandu where we reveled in what we had all just achieved.

Healthy and comfortable, John joined us in our celebration of the completion of our trek in the Khumbu.
Everest ER Docs Mackenzie, Watson and Koirala send an encouraging message to John following
his experience.
Case #2:
One morning, we woke up to another gorgeous day in the Khumbu. Every day of this trek was a bluebird day. After sorting out meds for various URI (upper respiratory infection) symptoms, we set out for Lukla on our final trekking day. About two hours into our walk, I received word that one of our trekkers fell and had back pain. Jim and I, along with Nim Dorji Sherpa, hiked back in sixth gear for about 20 minutes to find our friend in the excellent care of Deja, our soon-to-be first-year medical student at the University of Chicago. Deja presented the patient to me in an efficient organized manner so that we were caught up in 60 seconds. This was the first of many poignant moments over the next few hours. Deja's management and presentation demonstrated how much she learned from our lectures, discussions and scenarios along the trail. She impressed me beyond her level of training, especially her naturally calm, cool and collected demeanor.
Our trekker had pain, but luckily was neurologically completely intact in spite of what turned out to be a 30-foot fall, landing on her feet. Alena had fallen off the cliff-side of the trail when moving to make way for on-coming yaks and donkeys. We had a big debriefing on prevention and management after the fact, but in the heat of the moment, our team of physicians/trekkers/sherpas provided top notch and empathetic care to our fellow trekker, facilitating a helicopter rescue in under an hour. Clay, Sam and CJ as well as Pasang, Phula and Nim Dorji, worked with the litter. The chopper landing and take-off were award-winning.
Glen accompanied Alena to the Lukla clinic where there was chaos. Another poignant moment occurred during the clinic chaos. Glen, who is not in the healthcare field, raised his voice and asked, "Who is in charge?" When the attending physician identified himself, Glen said, "I only want to hear ONE voice - yours," pointing to the physician in charge. Glen had been listening to our trauma lectures as well. Alena was in good hands.
The main take-home point in prevention here is: always trek to the uphill side when passing yaks and donkeys on the trail. Alena had an L2 burst fracture with retropulsion into the spinal canal. She had surgery in Tokyo, and is now home in Osaka, with the spirited attitude that contributed immensely to her speedy recovery.

After a 30-foot-fall, we secured Alena to a litter and got her help with an excellent helicopter rescue. Photos appear with Alena's permission
The Wilderness Medical Society and Peak Promotions did something right - and the universe smiled upon us - in assembling a diverse, energetic, positive and warm group of trekkers, Sherpas and porters. Everyone brought something to the table. The group's dynamics progressed impressively quickly through Tuckman's phases of "Forming, Storming, Norming and Performing," though I'm not sure we will ever officially hit "Adjourning." Our chemistry was only enhanced by 17 days of perfect weather, trekking at the beginning of climbing season, and the amazing care with which Peak Promotions guided us. From the silly to the serious, laughter and perseverance were the glue that brought us together on our journey to reach Everest Base Camp and learn some wilderness medicine along the way.


While learning about wilderness medicine, our laughter and perseverance glued our group together throughout our successful journey trek to the Everest Base Camp.
